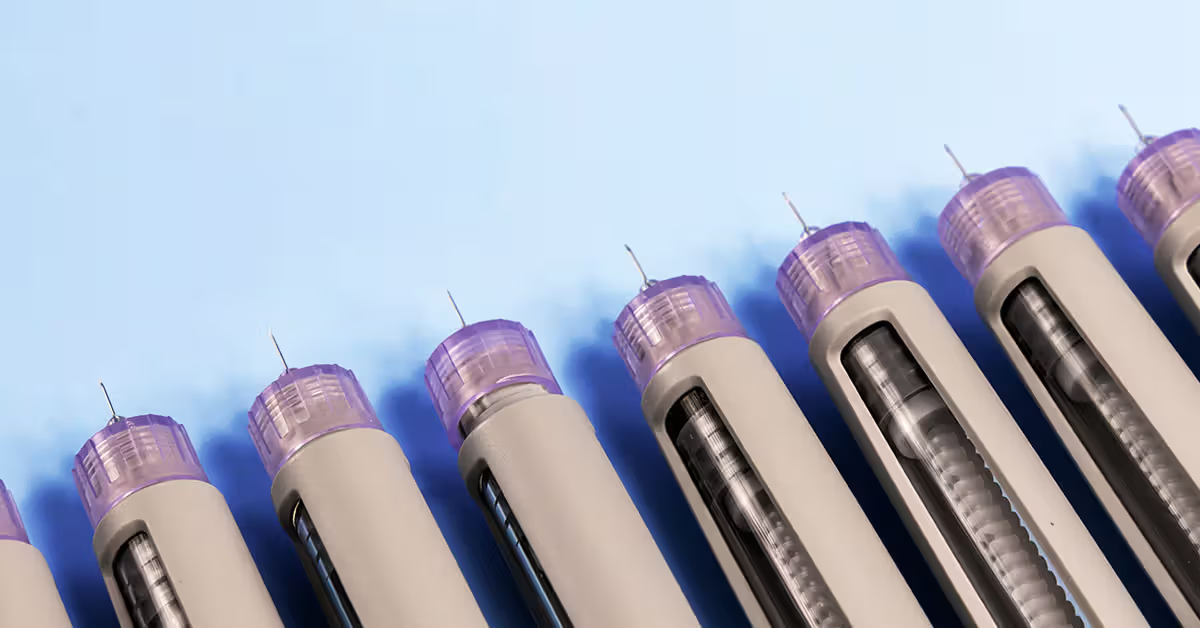
- GLP-1 receptor agonists, a class of medication used to treat type 2 diabetes and obesity, are sold under many brand names, including Wegovy, Ozempic, and Mounjaro.
- Although rare, these injections have been linked to a few side effects, including acute pancreatitis, or the inflammation of the pancreas.
- Following a recent rise in such reports, the UK has updated its guidance on weight-loss injections.
- Experts agree that this should not be a cause for alarm, but that people should be informed about this risk and the signs of pancreatitis to look out for.
GLP-1 agonists like Wegovy, Ozempic, and Mounjaro, which are used to treat type 2 diabetes and obesity, have been growing in popularity — so much so that in December 2025, the Food and Drug Administration (FDA) approved an oral pill form of Wegovy for weight loss.
However, as life changes as these medications have been for some people, they have also been linked to a few serious but rare side effects. One of these effects, which has come under scrutiny recently, has been acute pancreatitis.
The latest body to take action on this is the Medicines and Healthcare Products Regulatory Agency (MHRA) in the United Kingdom, which recently updated its guidance on these weight loss jabs, citing a rise in cases of acute pancreatitis reported to the Yellow Card scheme, which monitors adverse reactions to medicationyes.
Acute pancreatitis is the inflammation of the pancreas, presenting with symptoms such as sudden abdominal pain, nausea, and swelling. The patient information leaflets for drugs such as Wegovy, Ozempic, and Mounjaro state that pancreatitis is an “uncommon” side effect, affecting about one in 100 patients.
Data shows that 1.6 million adults in England, Wales, and Scotland used a GLP-1 medication for weight loss between 2024 and 2025.
In the UK, between 2007 and October 2025, 1,296 yellow card reports of pancreatitis linked to GLP-1 receptor agonists or dual GLP-1/GIP receptor agonists were reported, of which 19 were fatal.
Medical News Today spoke to three medical experts — Hector Perez, MD, a board-certified bariatric surgeon at Renew Bariatrics and an advisor at BestSurgeons, Mir Ali, MD, bariatric surgeon and medical director of MemorialCare Surgical Weight Loss Center at Orange Coast Medical Center in Fountain Valley, CA, and David Cutler, MD, a board-certified family medicine physician at Providence Saint John’s Health Center in Santa Monica, CA — about weight loss injections, their side effects, and how to spot signs of acute pancreatitis.
Pancreatitis risk with GLP-1s: Frequently Asked Questions
MNT.
How safe are GLP-1s?
“What this means for most people, is that if they do not stand to benefit significantly from GLP-1 medication the risks may very well exceed any potential benefits. For those without pre-existing pancreatic disease, GLP-1 medications are considered to have a favorable safety profile, with pancreatitis being rare and not definitively proven to increase in well-controlled trial data.”
—David Cutler, M.D.
gallstones
high triglycerides
heavy alcohol use
hypertriglyceridemia
metabolic syndrome
“Watch out for sudden, severe mid-epigastric pain that radiates to the back, pain that’s worse after eating or lying down, nausea or vomiting that doesn’t subside, and a tender or distended abdomen. Pain that doesn’t feel like typical (gastrointestinal) upset and is disproportionate to meals or exercise should be taken really seriously.”
—Hector Perez, MD
“The most common reactions are nausea, vomiting, diarrhea, abdominal pain, constipation, and gastroesophageal reflux. Less common reactions associated with these medications are medullary thyroid cancer risk, severe allergic reactions, and pancreatitis.”
GLP-1 drugs for weight loss, blood sugar management
brain fog
dulaglutide
liraglutide
semaglutide
tirzepatide
“I believe we should neither demonize these medications nor minimize real harm signals. The MHRA update is simply a reminder that powerful drugs require powerful surveillance, and until we have larger, long-duration real-world safety data, clinicians should err on the side of specificity in monitoring and patients should be taught exactly what to look for.”
—Hector Perez, MD